Critical Limb-Threatening Ischemia (CLTI)
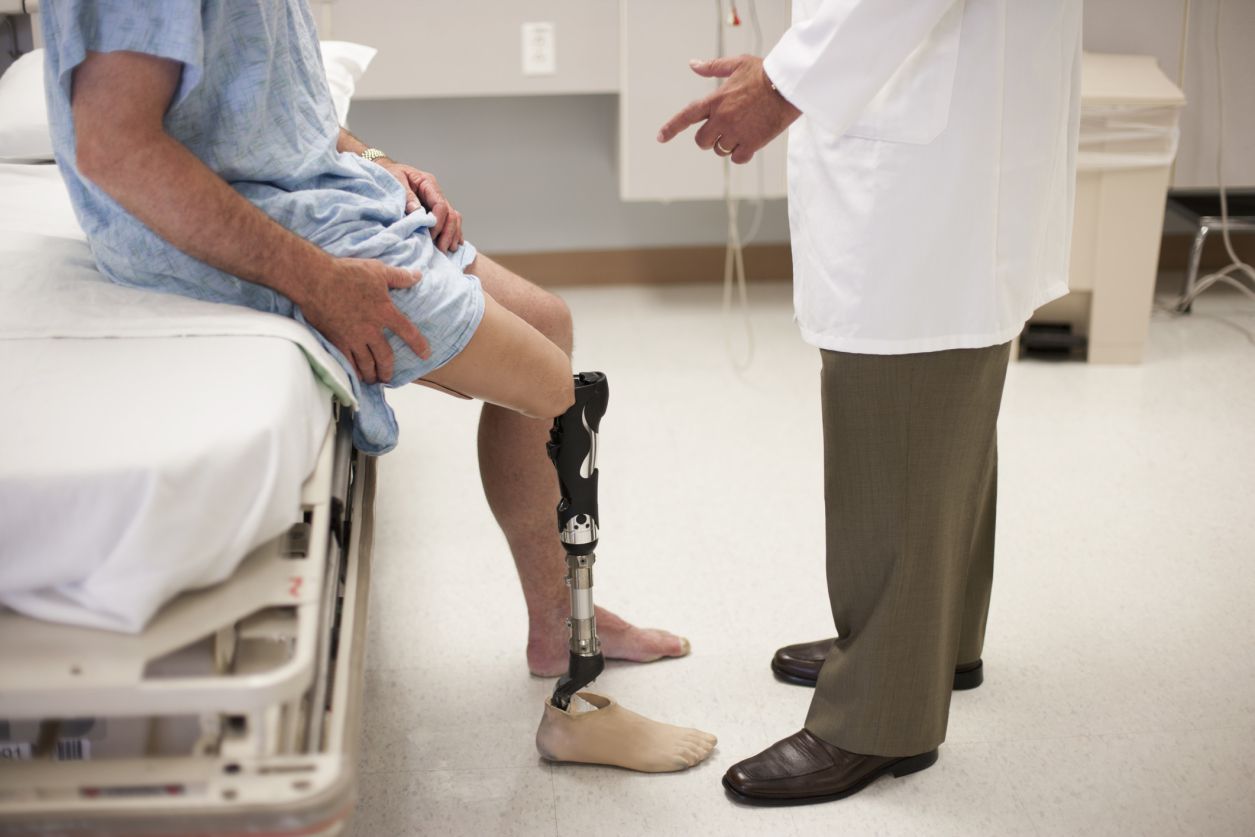
CLTI is the most severe form of peripheral artery disease, usually occurring in the feet or leg, and often leads to amputation. FreedomFlow® gives physicians a new way to treat these blockages and hopefully help more patients avoid this life-altering—and often fatal—outcome.
What is CLTI?
Peripheral artery disease involves the build-up of plaque in the arteries of the trunk, arms, or legs.
This plaque can eventually slow the flow of blood and thus oxygen to the affected part, and is often complicated by diabetes or heart failure, which can contribute to the reduced flow of blood to the feet and legs.
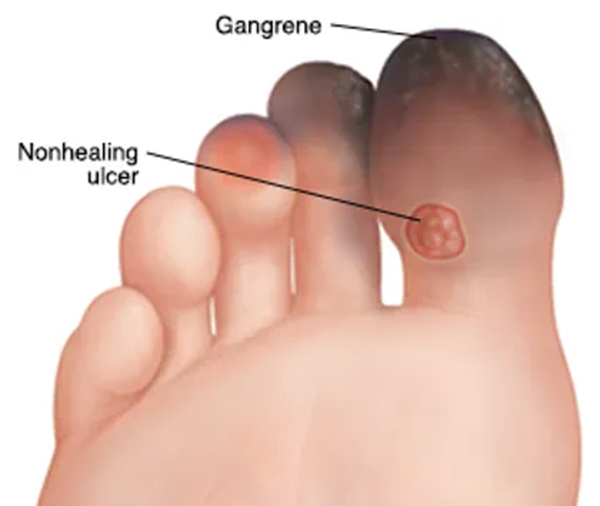
CLTI can have a serious impact on a patient’s quality of life, leading to chronic pain, wounds that don’t heal, sepsis, and gangrene.
Unfortunately this often leads to amputation, despite the fact that earlier intervention and less invasive treatment options—such as an atherectomy to clear the blockages—can help patients improve limb function, reduce pain, and avoid amputation.
What are the symptoms of CLTI?
How is CLTI diagnosed?
Various tests may be used to diagnose CLTI, such as:
- Tests to check the pulse and blood flow in the affected limbs – including an Ankle-Brachial Index (ABI), which compares blood pressure in the arms with that in the legs to see how well blood is flowing; a TBI or Toe Brachial Index measures the blood pressure in the toes
- Imaging – such as magnetic resonance imaging (MRI) and computed tomography (CT scan) to look for blockages in the arteries of the legs and feet
- Blood tests – to check for diabetes and high cholesterol
What causes CLTI?
CLTI and peripheral artery disease are caused by a build-up of plaque in the arteries. This plaque consists of fat, cholesterol, calcium, and fibrous substances in the blood.
Blockages in the arteries appears to stem from damage to the walls of the arteries in the heart, which may be due to a combination of:
- High blood pressure
- High LDL (“bad”) cholesterol
- Low HDL (“good”) cholesterol
- Smoking
- Diabetes or insulin resistance
- Obesity
- Sedentary lifestyle
- Inflammation
CLTI usually develops gradually over time in patients with a combination of conditions, especially diabetes and heart failure, that reduce blood flow to the feet and legs.
35-45% of patients go straight to amputation without CLTI diagnosis
How is CLTI treated?
Treatment usually aims to reduce pain, allow skin to heal, and improve limb function—which may include a combination of:
- Medication – to reduce blood cholesterol or high blood pressure, prevent blood clots, or treat pain.
- Angioplasty and stent placement – inserting a catheter into the blocked artery and inflating a balloon to press the plaque against the artery wall to improve blood flow; a stent (wire mesh tube) may be place to keep the artery open
- Atherectomy – inserting a catheter into the blocked artery and using a special device, such as Cardio Flow’s FreedomFlow®, to remove the blockage; it may be used prior to angioplasty and stenting if the plaque is especially hard to compress
- Bypass surgery – using a blood vessel from another part of the body to re-route or bypass the blockage
- Amputation – if blood flow cannot be restored, amputation may be necessary
How many people are affected by CLTI?
Peripheral artery disease is common in the United States, affecting some 8-10 million Americans, but only 10% of those will develop critical limb-threatening ischemia. Because CLTI patients are often hospitalized—often for bypass surgery or amputation—the condition has a serious impact on their quality of life and is costly for healthcare systems as well.
SOURCES: Joseph Karam and Elliot J. Stephenson, “Critical Limb Ischemia: Diagnosis and Current Management,” Journal of the Minneapolis Heart Institute Foundation, Fall/Winter 2017; Luigi Uccioli, et. al., “Critical Limb Ischemia: Current Challenges and Future Prospects,” Vascular Health Risk Magazine, April 2018, 14: 63-74; Scott Kinlay, “Management of Critical Limb Ischemia,” Circulation: Cardiovascular Interventions, February 2016, 9:2. Sources accessed online December 2020 and January 2021.